Abstract: The triad of robust state capacity, strong social trust, and competent leadership has been proposed as essential for a successful national response to the COVID-19 crisis. The flow of information among individuals and entities responsible for the response, and from them to the public, is the thread which unites and activates this triad itself. Effective response depends on timely and unambiguous information being openly available to government bodies, leaders, and society alike. Although Japan’s pandemic experience at the time of writing has been mercifully mild, the official Japanese response has objectively been quite flawed on many counts. What can be observed about the accessibility and transparency of the information concerning the pandemic that has been provided to the Japanese public?
As of early July 2020, the world is still in the midst of a pandemic which erupted in the first months of the year. Currently, in terms of infection and death rates, Japan appears to be faring better than most other nations, although many Asian countries, including South Korea, Taiwan, and Vietnam, have done consistently better (Roser et al 2020). But unlike these nations, the Japanese government has not yet implemented stringent or compulsory protective measures such as mandatory business closures or lockdowns, relying instead on relatively loose recommendations and voluntary compliance. On the one hand, the flexibility of the measures may be a positive characteristic, fostering a sense of civic responsibility rather than relying on coercion, but on the other this aspect also complicates any evaluation of the measures’ effectiveness. Neither the public nor the expert community can really judge which protective measures are proving effective or what the best approaches will be if the outbreak suddenly grows in size. In one sense, this is an uncertainty prompted by tenuous good fortune; at the moment, the entire Japanese nation seems to be doing something right. However, the uncertainty of the causes and durability of the apparent success calls into question the underlying rationale for government coronavirus policies and their implementation, as well as official communication efforts. Further, the uncertain basis of the positive trends obscures the need for greater transparency in decision making at all levels.
Seeing how few nations and regions have fared well overall during this pandemic, and indeed after any large recent disaster, perhaps we should consider the possibility that destructive events of this scale are too large for any society to truly handle adequately. Yet we have also seen how differences in preparedness and political leadership can result in huge disparities in the subsequent disruption, illness, trauma, and mortalities each population will suffer. Crisis response must address many constantly evolving challenges at once. Some challenges are technical, or in the current case, healthcare related. Logistical and personnel challenges can be immense. The task of coordination and messaging falls to government leaders, ideally assisted by a knowledgeable and responsible media. There has to be a plan, the people charged with implementing it must know it intimately and execute it well, and it must be quickly, frequently, and consistently communicated to the public. In all of these aspects the United States under President Trump has failed utterly and devastatingly, with large long-term negative consequences that are just beginning to unfold. But the official Japanese response has objectively been quite flawed on many counts as well, and yet the country’s experience so far has been much more fortunate.
Many observers have sought to identify factors which have enabled countries to limit the damage their citizens have suffered. Francis Fukuyama has recently proposed that state capacity, social trust, and leadership can be considered most important in this regard (Fukuyama 2020). This may be a useful rubric. “Countries with all three,” he states, “—a competent state apparatus, a government that citizens trust and listen to, and effective leaders—have performed impressively, limiting the damage they have suffered. Countries with dysfunctional states, polarized societies, or poor leadership have done badly, leaving their citizens and economies exposed and vulnerable.” Relative success to date has been experienced by both autocratic regimes and democratic ones, and both types of regime have also seen large failures. This suggests that the type of governance may be less important in this kind of crisis than its capacity and competence.
Fukuyama adds, “To handle the initial stages of the crisis successfully, countries needed not only capable states and adequate resources, but also a great deal of social consensus and competent leaders who inspired trust. This need was met by South Korea, which delegated management of the epidemic to a professional health bureaucracy, and by Angela Merkel’s Germany. Far more common have been governments that have fallen short in one way or another. And since the rest of the crisis will also be hard to manage, these national trends are likely to continue, making broader optimism difficult.”
This triad of robust state capacity, strong social trust (or perhaps social capital more broadly), and competent leadership does seem to be playing a major role in the worldwide response to COVID-19. What about in Japan? I believe we can observe these factors in play. To date, for a variety of justifiable reasons, the nation’s political leadership has been the target of most of the criticism, while strong social norms and compliance on the part of normal citizens is invariably credited at least in part for the tentative success experienced so far. The fundamental capacity of the state to respond to the outbreak, however, remains difficult to determine. It is obscured by layers of transparency-averse bureaucracy and generally poor messaging, and state capabilities, particularly their weaknesses, are rarely openly revealed and discussed by either elected leaders or bureaucrats. Even health experts encountered difficulty determining what the response plan was and who was responsible for executing its various parts. This important information is usually obscured in minute meeting notes, while public pronouncements have been marked by a vagueness and lack of detail, as well as major reversals of policy, which suggest that officials are making the plan up as they go along. I believe that the flow of information among individuals and entities responsible for the response, and from them to the public, is the thread which unites the capacity/trust/leadership triad itself. Good response depends on timely and unambiguous information being openly available to government bodies, leaders, and society alike.
It can further be argued that trust in government depends on transparency. The failures of the Japanese government and TEPCO in this regard following the Fukushima Nuclear Power Plant disaster in 2011 have been well documented and studied (NAIIC 2012). As the Fukushima disaster unfolded, official Japanese spokespeople often provided incorrect information, contradicted each other, and otherwise appeared untrustworthy to the public. Accurate information about the spread of radiation was not made available in a timely fashion, and when the public learned through the press or social media how much data showing the risks had been collected and not made available, either by intent or incompetence, they were outraged (Kasuta 2011). This disastrous and damaging experience should have been a cautionary lesson to emergency responders and policy makers everywhere. On one hand these failures are now considered textbook examples among emergency communicators worldwide of what to avoid and are frequently noted in workshops and conferences I have attended. Distressingly, though, similar patterns have emerged in many places, Japan included, in response to COVID-19. The lessons may not have been learned well enough.
This outrage and mistrust engendered in 2011 in Japan persists nearly a decade later. Counterintuitively, the Japanese COVID-19 experience may be an example of underlying mistrust in government being an adaptive psychology that can induce people to protect themselves better. The Japanese government’s response, notably the highly-visible fiasco of large scale outbreaks on the Diamond Princess cruise ship in Yokohama in February of this year, along with unconvincing assurances that everything was under control and a daily drumbeat in the media of distressing scenes from Wuhan, may have led many citizens to prepare for the worst early on. Already in January, Japanese nationals who had accompanied Chinese tourists on tours of Japan were reported to have contracted the virus (Teraoka 2020). More informed observers knew that pandemic protocols called for careful tracing of contacts in cases like these, to check every hotel, restaurant, and tourist spot the patients had visited in order to determine who else was present and so potentially at risk, and to encourage them all to isolate and be tested. The lack of public acknowledgement that this was being done at all, much less details about how it was being done and by whom, or reassurances that it was being done well, was worrisome. The way that the press apparently did not think to inquire about it either was worrisome as well. Based on the void of available information, the prudent assumption was that contact tracing was not being done, and that everyone should plan their own protection accordingly.
A key problem is that the public was given no visibility into what was actually happening aboard the Diamond Princess, or the government’s overall response. The press was ineffective as well. When Dr. Iwata Kentaro, an infectious diseases expert at Kobe University, posted a video online on February 18th in which he emotionally recounted what he saw aboard the ship in alarming terms, it garnered over 1.5 million views, confirming the worst fears of many (Iwata 2020). He later tempered his criticism somewhat. Government spokespeople eventually admitted that they were not well prepared to deal with the shipboard outbreak initially, but that the eventual national pandemic response plan — so-called “cluster countermeasures” — was largely based on epidemiological analysis of the rates of viral transmission observed there (Jimi 2020). The Diamond Princess appears to have been a petri dish-like incubator of both the coronavirus and clumsy attempts to control information.
Crisis communicators are trained in several key principles which, if executed well, can help assure calm cooperation from the public with bothersome protective measures. Communicators are advised to have a clear plan of action beforehand, and a well thought-out pre-prepared script of messages that can be quickly tailored to the specifics being dealt with. Sophisticated crisis information websites should be built well before they are needed, and carefully tested, with applicable boilerplate text and images and placeholders where the specifics can be added. Communicators are taught to begin their messaging within hours, if not minutes, of the first reports of a disaster, even if it is only to say, “We are aware of these reports and are engaged and will be back quickly with more information. Here is our disaster response website.” Messaging must be consistent, without contradiction, but should acknowledge what is still unknown. It has to be presented through as many different channels as possible, including frequent and well-publicized press conferences, traditional media, and social media. Furthermore, the spokespeople must be carefully selected for their public speaking skills and charisma and carefully trained for the job. They should rehearse constantly using different scenarios. Political leaders have an important role in crisis messaging, to express concern and compassion, and to project calm and competence. But they should let the trained experts carry the bulk of the message to the people (Bonner and Brown 2020).
None of this was evident in Japan in 2011, and it has not been evident in 2020 either. Governor Koike Yuriko of Tokyo is a rare exception. Multilingual and with a background as a television announcer, she has demonstrated competence as an official communicator to both the Japanese and non-Japanese communities under her jurisdiction. Similarly, her government produced the most informative and user-friendly official website in Japan for COVID-19 issues, which is also multilingual (Tokyo Metropolitan Government 2020). Eventually, a handful of specialists, such as Dr. Nishiura Hiroshi of Hokkaido University, a key member of the Ministry of Health’s Cluster Response Team, achieved name recognition and familiarity to the Japanese public, becoming a de-facto “trusted” communicator nicknamed “Uncle 80%” for his repeated recommendation that the pandemic could be tamed if everyone reduced their social contacts by that percentage. But by and large, the public has been informed not by skilled experts but by TV talking heads, sound bites, and lengthy, droning televised press conferences given by unprepared and unconvincing middle-aged male politicians and bureaucrats. None of them have inspired trust. On the contrary, poor messaging seems to have led to a widespread sense of unease and abandonment among the populace in the first months of the outbreak. Not surprisingly, in response many people have relied more on social media gossip instead, as they did in 2011. People can feel connected and listened to on social media in a way they cannot with the official messaging. Social media provides compassion and community, which are essential for coping with crises, as well as an outlet for anger and outrage.
Likely due the information vacuum and the sense of abandonment, rumors became rampant in Japan from the earliest weeks of the pandemic. These were not only about the virus itself and its health consequences, but about its effects on travel, lifelines, business, and the ability to take adequate precautions. Though experts initially said they are of little help, face masks became unavailable in Japan for months, as did hand disinfectant. There was a nonsensical run on toilet paper, as there has been in Japan following every crisis since the oil shock of 1973. Travelers were especially concerned about becoming stranded, and answers about possible quarantines when traveling to Europe, the US, or other countries were long in coming. Trustworthy government spokespeople should have started explaining when and why such steps might be taken, and for how long, during the first weeks of the crisis. Instead, the often unpleasant news arrived in media reports based on statements from foreign governments instituting travel advisories. As of this writing, the shoe is on the other foot, with the Japanese government announcement of a poorly explained and indeterminate ban on non-Japanese, even residence card holders, returning to Japan (Osumi 2020b). With little prior consultation with either the education community or local governments, and no preparation, Prime Minister Abe announced nationwide school closures on February 27. This caused a crisis for both daycare and working parents, who received no word of what kind of compensation or assistance would be available or when. It was clear that the Prime Minister was doing all he could to help ensure that the 2020 Tokyo Olympics would be held as planned, and this caused justified suspicion about the nation’s slow response. As in 2011, the lack of trustworthy information spawned fast-traveling conspiracy theories which are easily debunked but remain in wide circulation regardless. Many people concluded that people in government prioritized minimizing their own political risks over helping the public deal with their valid health concerns.
Citizens expressed concern and outrage, particularly about the unavailability of testing. Compared to countries which quickly rolled out intensive COVID-19 screening and testing programs, like South Korea, Japan has not done much surveillance testing to date. As of July 4th, 2020, Japan’s total number of PCR tests stood at just 348,000, or 0.27% of Japan’s population (Wingfield-Hayes 2020). In terms of percentage of the population tested, Japan has consistently been lower than other developed nations, particularly when compared to its Asian neighbors. Widespread public concern emerged by March 2020 that the lack of testing obscured a much wider incidence of coronavirus which was not being detected. This concern focused on uncertainties regarding the degree of spread of the virus by asymptomatic or pre-symptomatic carriers — those who contract the virus but experience no physical symptoms of illness, like coughing or fever (Li et al 2020). If they have no symptoms that induce them to seek testing, there is a higher risk they will unknowingly infect others. At the same time, many people who experienced symptoms and were concerned they might have the virus found it impossible to get tested.
The policies regarding testing remain obscure and difficult for average citizens and even researchers to find and understand (Brown 2020a, 2020b, 2020c). In fact, it was difficult for outside observers to determine which bodies are actually responsible for testing. Eventually it became clear that testing for the virus in Japan had been intentionally limited by official policy. Japan has no official body like the US CDC, or similar agencies in South Korea, Taiwan, and many others that is tasked with handling emergency public health issues. Instead, the National Institute of Infectious Diseases (NIID), under the Ministry of Health, Labor, and Welfare (MHLW) is tasked with collating and analyzing epidemic and pandemic data (NIID 2020). It uses a system called the National Epidemiological Surveillance of Infectious Diseases (NESID), which was established in 1981 as part of the Infectious Disease Surveillance Center (IDSC) (NESID 2020). Due to the complexity of this system, and the difficulty of modifying how it operates, it moves cautiously and slowly, and is not very adaptable under the stress of new outbreaks like we are seeing with COVID-19. In practical terms, this means that data sources which have been part of the system for a long time, particularly public health institutions, are prioritized over others, regardless of their actual relevance to emergency response. Reporting criteria are fairly fixed and difficult to change. A lot of the issues surrounding COVID-19 case data collection and reporting we continue to observe in Japan appear to be the result of the system working as it was designed to. It is neither agile nor flexible.
|
Fig. 01: Consultation procedure flowchart provided to Japanese residents seeking COVID-19 testing, English language version (Source: Tokyo Metropolitan Government) Click to expand. |
All requests for COVID-19 testing must be approved by the NIID, which has been overloaded for several months. Although there was some relaxation in the succeeding months, testing requirements publicized in March 2020 stipulate many conditions that need to be met before testing will be made available (Fig. 01). In order to qualify for the first medical consultation, a person must have been in close contact with a known infected person, defined as contact over a long period of time or living together, examining or caring for a patient without taking protective measures, or contact with bodily fluids, and currently have fever of 37.5’ Celsius or respiratory symptoms, and/or had visited an endemic area in Hubei or Zhejiang Provinces, and currently have fever of 37.5’ Celsius or respiratory symptoms. Those who call Japan’s Novel Coronavirus Patient Consultation Call Center and are recommended for in-person outpatient consultation must then appear at the designated center and be examined. If the doctor suspects COVID-19, he can recommend a PCR (polymerase chain reaction) test and seek approval from the NIID for testing. In practice, we are told, the NIID is so inundated with requests it is often difficult for doctors to get through by phone. This system presents a strong bottleneck to testing.
As is unfortunately often the case, it is difficult for average citizens to understand or navigate this system and its requirements, and many became quite frustrated and alarmed. This has been an extremely weak link in the information needed to instill trust. If they’re feeling ill with similar symptoms, residents want to know how serious their prognosis is. Some journalists eventually sought to clarify the testing policy for the public. An article in the Nikkei Asian Weekly from March 12, 2020, for instance, attempted to explain the policy (Yano 2020). The capacity is there, the writer noted, and the number of tests has been limited because the Ministry of Health, Labor and Welfare wanted the data to support an epidemiological investigation, not for medical care. In particular, the policy focuses on identifying clusters of the disease, to help in the allocation of medical resources. This is also emphasized in official policy documents from February of this year, available at the MHLW website:
|
Establish the surveillance system to grasp the epidemic situation in Japan, while switching to use of PCR test for the confirmation of diagnosis necessary to treat pneumonia patients who require hospitalization, in communities where the number of patients continues to increase. The local government shall use active epidemiology surveys to identify a cluster based on individual patient outbreaks in cooperation with the Ministry of Health, Labour and Welfare and experts, and request the necessary measures including closure of the related facilities and voluntary restraint of events if there is a possibility that such a cluster exists (MHLW 2020). |
Health Ministry staff felt that surveillance testing must be adequate for understanding the scale and geographical distribution of the outbreak, but that too much testing, particularly of the “worried well,” would overwhelm the healthcare system. Notably, the government initially decided against allowing rapid test kits developed by overseas pharmaceutical companies to be used in Japan, fearing that the variability of test results would hamper nationwide epidemiological analysis. After criticism, the criteria were relaxed, and testing capacity and test numbers themselves began to increase (Osumi 2020a).
This testing policy, so unlike the intensive large-scale programs proven successful in nearby countries, was a gamble, and it was extremely poorly communicated at the time. That no-one in government took center stage to explain it to the public, to “own” it, in March or April, may be an indication that they considered failure to be likely, and preferred to avoid being associated with it. Clear public discussions of the policy and its implementation only came later, in recent months, as policymakers and advisors sensed public relief at relatively low nationwide case numbers. Dr. Saito Tomoya, director of the Department of Health Crisis Management at Japan’s National Institute of Public Health, gave well-publicized interviews for Japanese and overseas media in June 2020, to explain what the Japanese government had done and why. Much of the public heard for the first time that 69 local public health centers in Japan, with more than 25,000 staff trained in contact tracing, had been laboriously “calling patients and politely asking them to name the people they have met with in the last fortnight” (Saito 2020). He described this regressively low-tech aspect of the system, as well as the obscure overall policies, as working effectively. He also claimed, despite the abundant contrary evidence, that the government had demonstrated a “capability to share knowledge about the disease with the public in an easy-to-understand manner.” The Prime Minister and others echoed similar talking points. It amounted to a politically motivated victory lap, and was likely premature.
|
Fig. 02: Japanese government poster urging avoidance of the “Three Cs,” English language version (Source: MHLW) |
A nail-biting increase in nationwide cases became evident in mid-March 2020, and the daily count increased to a peak of over 700 cases on April 11. Heeding the advice of the official committees, the Abe administration declared a state of emergency for Tokyo and the prefectures of Kanagawa, Saitama, Chiba, Osaka, Hyogo and Fukuoka, beginning on April 8. This was initially intended to last one month, but was eventually extended to two and spanned the entire nation, finally lifting on May 25. Because the Japanese government does not have the legal authority to implement compulsory measures such as lockdowns and curfews, Abe’s emergency declaration depended upon voluntary preventive measures, such as the closure of stores and restaurants, staying home, avoiding unnecessary travel, mask wearing, and personal hygiene. The only highly visible messaging concerned avoiding the “three Cs” — closed, crowded spaces with close contact (Fig. 02). Preventing this specific behavior was promoted through media, online graphics, and actual printed posters.
|
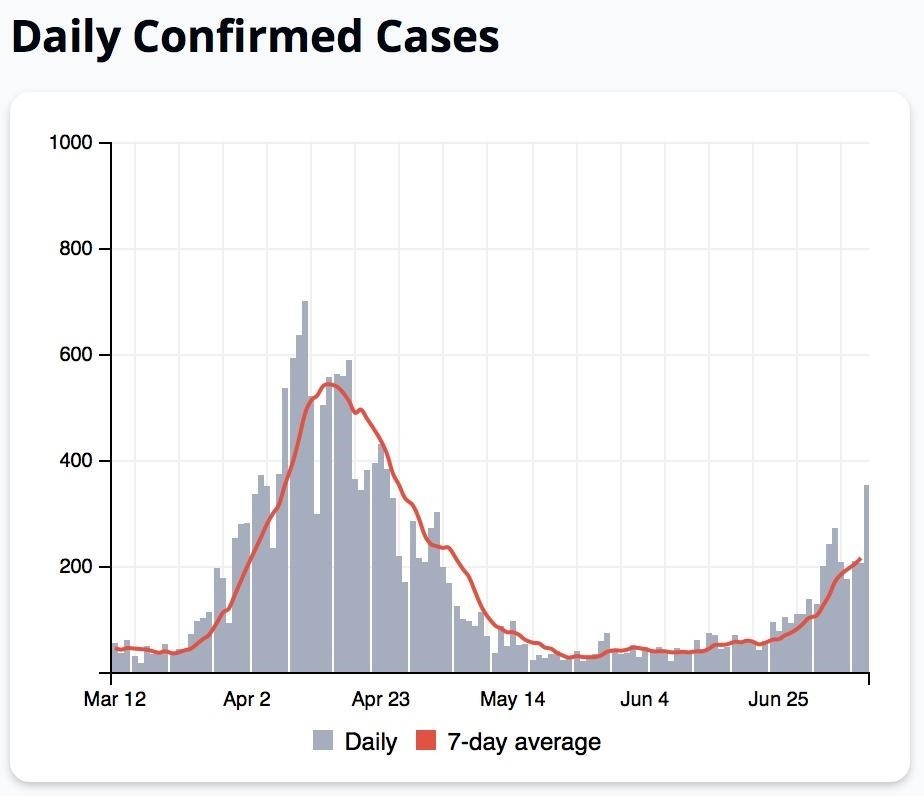
Fig. 03: Japan COVID-19 confirmed cases, March 12-July 9, 2020 (Source) |
A steady decline in cases followed the initiation of the state of emergency, to a seven-day average of about 30-50 cases per day nationwide from mid-May through mid-June. In recent weeks, as the emergency was lifted, more schools reopened, and many individuals relaxed their preventive vigilance. Not surprisingly the case numbers have increased again. In the week prior to July 9, 2020, there were six days with over 200 cases. This is very worrying, and clearly evident in data graphs (Fig. 03). Nevertheless, so far it is a small increase compared to what is occurring in many other parts of the globe. It’s possible, then, that there has been (barely) enough testing in Japan to allow public health specialists to anticipate the eventual spread of the virus, to prepare the necessary hospital beds, and to slow the spread of contagion. But as leading public health specialist Dr. Kurokawa Kiyoshi wryly noted in a personal communication, “Nobody knows.” Nevertheless, many voices have been declaring victory in Japan over the coronavirus since at least March 2020. The fact is, researchers are only now, in June and July, getting a good idea of what the actual viral transmission situation was like in Japan from January to April (Furuse et al 2020).
Reassuring the public and reinforcing confidence in public institutions is a valid goal of crisis messaging. But if the messages run counter to public experience or are overlaid onto information flows marked by a lack of transparency, then they will not be believed, and the sources will not be trusted. This is one reason why it is extremely risky to declare victory too soon, especially with a viral pandemic which is expected to continue for over a year in successive waves. As early as March, when Italy and New York were in the midst of coronavirus-induced healthcare system overloads, the caseloads in Japan were much lower. As questions emerged around the lack of testing and the possibility that a large number of cases were being missed, there was a chorus of “boosters” who, disregarding the immense uncertainties, were already claiming that Japan had beaten the virus. Most pointed to good hygienic norms, such as handwashing and mask wearing, as the secret of Japan’s apparent success. Others went so far as to claim that the government and health care leaders had accurately gauged the problem and implemented a well thought out (but evidently practically secret) plan. As case numbers grew rapidly into mid-April, the chorus of “success” seemed to have quieted, only to re-emerge a few weeks later as the numbers temporarily stabilized at a lower level (Omi and Oshitani 2020).
This urge to prematurely claim victory has not been limited to Japan of course. But it has brought with it a competitive current in media, which seems to be covering the pandemic as if it were sports. Rather than focus on helping the public understand and deal with the great uncertainties the pandemic presents in almost every aspect, there has been a detectable desire on the part of many journalists to declare “winners” and “losers.” Who was right about how bad it would get, and who was wrong? Unlike any past pandemic or other crisis in recent memory, COVID-19 has occasioned a blossoming of data journalism. There are a number of outstanding internet-based data collation and visualization projects, and they have become increasingly “friendly” and accessible for the general audience (Roser et al 2020). But despite the great detail contained in the available data, it is still insufficient for helping us determine with confidence what will happen going forward. Good data journalism illustrates and highlights these uncertainties. Good epidemiologists acknowledge them as well, while government spokespeople in Japan tend to speak with unwarranted self-congratulation and certainty.
Despite the reassuring overall trends in Japan so far, some of the greatest caution has been expressed by leading Japanese epidemiologists. Dr. Shibuya Kenji, Director of the Institute of Population Health at King’s College in London, is known for his objectivity and frankness, evident during the Fukushima thyroid cancer screening controversy a few years ago. Early in the pandemic he raised cautions about the risks of relying exclusively on the “cluster countermeasures” approach and has urged a much larger expansion of testing in Japan (Shibuya 2020). If much more extensive testing was being done, he noted, particularly of asymptomatic and pre-symptomatic cases, we would have a fuller and more current picture of the spread. He has noted reasons why it is difficult to draw many firm epidemiological conclusions from the data we are given, including inconsistent and delayed reporting of tests done at private labs. He pointed out the time lag between the onset of infection and the appearance of symptoms in an individual, and of the additional time lag before any case is diagnosed as positive. Most concerningly, none of the relevant data is publicly available, so outside researchers have no way to independently validate, replicate, or scrutinize it. Shibuya himself was unable to obtain COVID-19 data from Japan’s National Institute for Infectious Diseases (NIID) to analyze, which should be a very straightforward process, particularly for a researcher of his status and reputation. Without access to the background dataset, we are stuck with understanding very little from the publicly available data.
The success South Korea has had so far in minimizing the spread of COVID-19 within its borders, according to Shibuya, is because they focused on the basics: to test and isolate. Because of their bad experience with MERS and SARS in earlier years, they were well prepared for this outbreak. We can say that the same is true for Taiwan. Japan’s focus on border control and identifying clusters of major symptoms, — “cluster countermeasures”— misses asymptomatic or pre-symptomatic mild cases thus facilitating community and hospital transmissions. The country needs to be conducting 100,000 tests per day regardless of the current case counts, and Shibuya believes this goal is achievable. Without this we cannot have confidence that a much larger and less controllable outbreak will not appear at some point. In another press conference, Dr. Nishiura was more sanguine. His stated opinion is that even if testing is increased to 20,000 per day, the public health response will still be limited by the capacity of health care facilities. Because of personnel issues, logistics, and other issues, he noted, “The reality is we do not have the capacity to do what Korea has been doing with intensive testing and tracing” (Nisihura 2020). This was a rare admission of a lack of crucial state capacity, and acknowledgement that Japan’s response has been hobbled.
The currently reassuring low Japan case count notwithstanding, based on known asymptomatic-to-symptomatic case ratios from other countries, both Shibuya and Nishiura believe that the number of actual infections is at least ten times what is being reported. This has not changed since March. Results of modeling done by Dr. Nishiura, which reportedly played a large role in persuading Prime Minister Abe to order the State of Emergency in early April, estimated that without strong countermeasures the number of serious COVID-19 cases in Japan could reach as many as 850,000, and the death toll as high as 400,000 (Swift 2020). Largely because the public was scared, it cooperated with the countermeasures and modified their behavior, and so these tolls have not come to pass. But as the current experience of many US states and in other countries proves, large outbreaks can emerge after months of more manageable levels. Because of this, the uncertainties remain, and these estimates have not lost relevance. Nevertheless, on May 16, a Tokyo-based journalist with a major foreign news agency, noting that Safecast had reported Shibuya’s and Nishiura’s worst-case estimates, crowed on Twitter, “Fortunately, quite a big weekly average increase required to get to the 850,000 cases in Japan and 400,000 deaths that Safecast predicted a couple of weeks ago…at the current rate they will be right in 11,600 days” (Carter 2020). We replied that Safecast’s information policy is to carefully report what various experts say and try to put it into context, which includes attempting to characterize the uncertainties and the caveats. It was precisely the plausibility of the high expert estimates that motivated Abe to declare the emergency, thereby bringing the case count down. Safecast additionally noted that although the situation in Japan appears reassuring now, COVID-19 data is very uncertain in general, with many blind spots and inadequate policies and implementation. This journalistic exchange underscored that even otherwise well-educated people in the “information” profession are often not equipped, be it intellectually or emotionally, to deal with scientific uncertainties associated with matters of life and death. Unfortunately, this failure to grasp and convey the many uncertainties surrounding COVID-19 has been a consistent weakness of much media coverage of the pandemic in Japan and elsewhere.
What should we expect in the coming weeks and months? Again, nobody knows. In terms of the kind of clear, prompt, and open information upon which the effectiveness of the capacity/trust/leadership triad hinges, in Japan there may have been some incremental improvement, particularly on the part of regional and local governments, but it was followed by a retreat into the non-transparency default mode. On the one hand, more and better information from both official and independent sources has become available and proven its utility (Reustle 2020). But official messaging is still inconsistent and overly rosy, and reveals a largely reactive, as opposed to proactive, approach. The public, for its part, having seen the numbers go down after having dutifully worn masks, washed hands, and avoided crowded places for weeks, and nervously watched them rise again as everyone relaxed, now grasps, if incompletely, its own influence on public health. Citizens also seem to have settled into a wary “trustlike” truce with the government and with each other about COVID-19. But few would claim to understand well either the testing system parameters or how it was decided and implemented. They do know, however, that they should not count on a test being available for them or their family members anytime soon, because they are being “saved.” We cannot exclude the possibility that Japan might yet experience an exponential growth in cases, but no one can quantify the likelihood. In the face of the continuing uncertainties, we would urge the government to assume the worst and ensure that necessary social, medical, and economic support will be easily available when needed.
Sources
Bonner, S., Brown, A. (2020) ‘What the Fukushima meltdowns taught us about how to respond to coronavirus’, Bulletin of the Atomic Scientists, 13 March. (Accessed: 5 July 2020)
Brown, A. (2020a) ‘COVID-19 Testing in Japan: The situation and ramifications’, Safecast Blog, 17 March. (Accessed: 5 July 2020)
Brown, A. (2020b) ‘Making sense of COVID-19 numbers in Japan’, Safecast Blog, 24 March. (Accessed: 5 July 2020)
Brown, A. (2020c) ‘Uncertainties about Japan’s COVID-19 data’, Safecast Blog, 28 April. (Accessed: 5 July 2020)
Carter, S. (2020) ‘Fortunately, quite a big weekly average increase required to get to the 850,000 cases in Japan and 400,000 deaths that Safecast predicted… a couple of weeks ago…at the current rate they will be right in 11,600 days…’, [Twitter] 16 May. (Accessed: 5 July 2020)
Fukuyama, F. (2020) ‘The Pandemic and Political Order’, Foreign Affairs (July-August) (Accessed: 5 July 2020)
Furuse, Y., Sando, E., Tsuchiya, N., Miyahara, R, Yasuda, I., Ko, Y.K., et al (2020) ‘Clusters of coronavirus disease in communities, Japan, January–April 2020’, Emerging Infectious Diseases 26(9) (Accessed: 5 July 2020)
Iwata, K. (2020) ‘Aboard the Diamond Princess’, Foreign Correspondents Club of Japan,20 February. (Accessed: 28 June 2020).
Jimi, H., Hashimoto, G. (2020) ‘Challenges of COVID-19 outbreak on the cruise ship Diamond Princess docked at Yokohama, Japan: a real-world story’, Global Health & Medicine, 29 April. (Accessed: 5 July 2020)
Katsuta, T. (2011) ‘Genpatsu no hokusei 30 kiro takai hoshasenryo’, Asahi Shimbun, 24 March, p.2.
Li,R., Pei, S., Chen, B., Song, Y., Zhang, T., Yang, W., Shaman, J. (2020) ‘Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV-2)’, Science, 368(6490) pp. 489-493. (Accessed: 5 July 2020)
MHLW (2020) ‘Basic Policies for Novel Coronavirus Disease Control’, February 25. (Accessed: 5 July 2020)
NAIIC (2012) The Official Report of the Fukushima Nuclear Accident Independent Investigation Commission: Executive Summary. National Diet of Japan, Fukushima Nuclear Accident Independent Investigation Commission.
Infectious Disease Surveillance Center, National Institute of Infectious Diseases (2018) ‘Infectious Disease Surveillance System in Japan’, February. (Accessed: 5 July 2020)
National Institute of Infectious Diseases (2020) ‘Infection control for COVID-19’, 21 February. (Accessed: 5 July 2020)
Nishiura, H. (2020) ‘Kansen-sha wa happyō no `sukunakutomo 10-bai koeru’ Hokudai kyōju, Keidai byōin jirei mo `kichōna jōhō’’, The Page, 24 April. (Accessed: 5 July 2020)
Omi, S., Oshitani, H. (2020) ‘Japan’s COVID-19 Response’, 1 June. (Accessed: 5 July 2020)
Osumi, M. (2020a) ‘Will Japan’s virus testing policy be enough to flatten the curve?’, Japan Times, 16 March. (Accessed: 5 July 2020)
Osumi, M. (2020b) ‘Foreign residents stranded abroad by Japan’s coronavirus controls’, Japan Times, 25 May. (Accessed: 5 July 2020)
Reustle, S. (2020) Japan COVID-19 Coronavirus Tracker. (Accessed: 5 July 2020)
Roser, M., Ritchie, H., Ortiz-Ospina, E., Hasell, J. (2020) Coronavirus Pandemic (COVID-19), Our World in Data (Accessed: 5 July 2020)
Saito, T. (2020) ‘Contact-tracing and peer pressure: how Japan has controlled coronavirus’, The Guardian (International) 6 June. (Accessed: 5 July 2020)
Shibuya, K. (2020) Online Media Briefing: Kenji Shibuya, 23 April. (Accessed: 5 July 2020)
Swift, R. (2020) ‘Japan health ministry projects 400,000 deaths without virus containment measures: media’, Reuters, 15 April (Accessed: 5 July 2020)
Teraoka, A. (2020) ‘Japanese driver of Chinese tourist bus contracts coronavirus’, Nikkei Asian Review, 28 January. (Accessed: 5 July 2020)
Tokyo Metropolitan Government (2020) Updates on COVID-19 in Tokyo (Accessed: 5 July 2020)
Wingfield-Hayes, R. (2020) ‘Coronavirus: Japan’s mysteriously low virus death rate’, BBC News, 4 July. (Accessed: 5 July 2020)
Yano, H. (2020) ‘Coronavirus: Why Japan tested so few people’, Nikkei Asian Weekly, 12 March. (Accessed: 5 July 2020)